Specialty CL research review
Ortho-k for myopic progression prevention in children
Vanderveen DK et al. Ophthalmology 2019; 126:623-636
Review: This extensive review paper provides a meta-analysis of 13 of the ‘best’ papers (from 162 citations) to evaluate the ability of orthokeratology (ortho-k) treatment to reduce myopic progression in children and adolescents, compared with the use of spectacles or daytime contact lenses (CLs) for standard refractive correction.
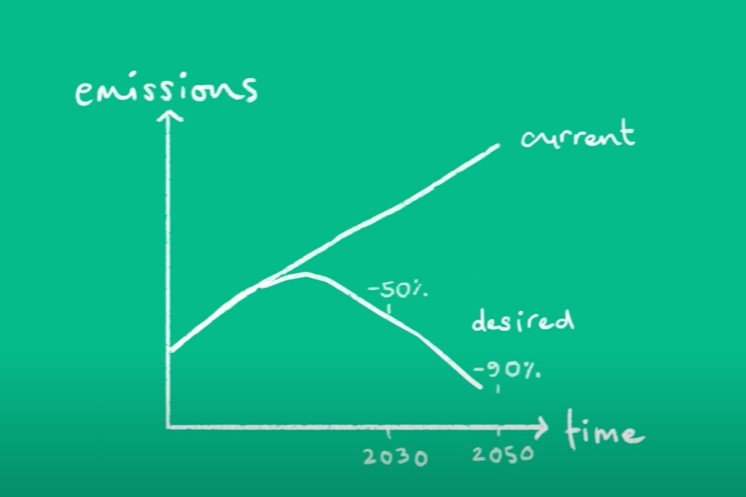
Ten of the 13 studies used change of axial length as the primary measure. The other three papers used change in refraction. Most studies were performed in populations of Asian ethnicity. Over the average study period of two years, ortho-k typically reduced axial elongation by about 50% - a change of 0.3mm for ortho-k, compared to 0.6mm for control patients. This corresponded to a typical difference in refraction of approximately 0.5 dioptres. They also ascertained that younger age groups and individuals with larger pupil sizes may enjoy a greater effect with ortho-k.
Myopic rebound/regression upon discontinuation of ortho-k was only studied in one paper and remains an unanswered question. The estimated rate of microbial keratitis (MK) in ortho-k has only been reported in one study: 7.7 cases per 10,000 patient-years, which is similar to other overnight CLs. Attributable risk factors included poor practitioner skills/systems and patient non-compliance.
Comment: Overnight ortho-k has become very popular in Australasia. It provides a convenient ‘dual action’ of clear unaided daytime vision, due to overnight central corneal flattening, and myopia control, presumably provided by the steeper mid-peripheral moulded corneal shoulder as well as improved accommodation function. Some parents of ‘high risk’ children also request combined ortho-k and atropine therapy in the hope of even better myopia control. Recent studies support this synergistic model in providing a further 50% reduction in increased axial length compared to ortho-k alone.
All children/adolescents wearing overnight ortho-k CLs require heavy supervision and regular check-ups. This can be labour-intensive for the family and their practitioner. Central corneal NaFl staining is unacceptable and the CLs must be kept meticulously clean. At least twice-yearly follow-ups are recommended over the long term and often the practitioner will need to either professionally clean or replace the CLs on a regular basis.
Scleral CLs for ocular surface disease - patient selection and special considerations
Harthan JS & Shorter E. Clin Optom 2018; 10:65-74
Review: This article summarises the benefits of large diameter rigid gas-permeable contact lenses (CLs) to vault the cornea and bathe it in a tear reservoir. Corneal hypoxia, however, remains a risk so the lens material and tear film thickness combined must have a high Dk/t for adequate oxygen transmissibility. As per the Tear Film and Ocular Surface Society (TFOS) Dry Eye Workshop II (DEWS II) report, individuals who are symptomatic with signs of ocular surface disease, as well as those with neurotrophic conditions who have signs of ocular surface disease without symptoms, are excellent candidates.
For challenging medical conditions, scleral lenses can be used in combination with other therapies (such as topical lubricants, punctal occlusion, cyclosporine, tarsorrhaphy) to delay or prevent surgery whilst also providing optimal visual correction. Listed conditions include Sjögren’s syndrome (SS), exposure keratopathy from eyelid malposition, persistent epithelial defects (PEDs), neurotrophic keratopathy, limbal stem cell deficiency, and graft-versus-host disease (GVHD). Any associated meibomian gland deficiency also needs to be managed. To improve lens wetting and prevent fogging, alcohol-based lens cleaners, HydraPeg surface coatings and toric periphery lens designs can be used.
Comment: Therapeutic soft CLs, which may be cheaper and easier to fit than scleral CLs, can protect the corneal surface from the eyelids in cases of recurrent erosion syndrome (RCES), Fuchs’ endothelial dystrophy and bullous keratopathy. Disposable silicone hydrogel (SiHg) soft CLs can be worn overnight for short periods, and frequent replacement reduces the risk of lens-induced keratitis. Overnight wear of scleral lenses runs the risk of corneal hypoxia but, unlike soft lenses, they can provide a tear reservoir to bathe the cornea for long periods during the day, whilst also neutralising any corneal irregularities.
Combining optics and comfort: piggyback and hybrid CLs
Sherman S and Wilson N, Review of CLs Sept/Oct 2017 18-21
Review: With the recent surge in popularity of scleral CLs, it is easy to forget that piggyback and hybrid CL systems can also be good troubleshooters on irregular corneas. If an RGP lens is uncomfortable and/or poorly centred, slipping a disposable soft lens under it can often alleviate some of these issues by acting as a cushion between the RGP lens and cornea. Also, eyelid sensation can be reduced if the RGP lens moves less over the soft piggyback. High Dk silicone hydrogel soft CLs of a low power (+/- 0.50) will have no effect on the RGP optics, but may require a slightly flatter RGP base curve for the best fit. Patients, however, must be prepared to invest in the time and money associated with a two-lens system. Also, the soft lenses may flute off at the edge on steeper corneas.
Hybrid CLs have improved rapidly since their introduction in 1985. The early versions suffered from splitting at the bonded hard/soft junction and the materials were also low on oxygen transmission. The current generation (Duette and Ultrahealth) have a high Dk (130) rigid centre and a silicone hydrogel soft skirt of Dk 84. However they cannot correct residual (lenticular) astigmatism, and are still prone to dryness and protein deposition. Corneal staining from the RGP centre is a common problem and the lenses need to be kept meticulously clean with systems such as hydrogen peroxide and should be replaced twice a year. Hybrid lenses can also be more difficult to remove than soft/piggyback systems.
Comment: In my experience, hybrid CLs can be challenging to fit correctly (high molecular weight fluorescein and a written yellow filter help) and the soft skirt can tighten up over more hours of wear. In comparison, although piggyback systems are less convenient for the patient to manage, they probably have a lower complication rate. Tightly fitted hybrid CLs can be associated with limbal vessel changes and the cornea can also suffer from poor tear exchange. Further improvements in hybrid CL design and materials are thankfully on the horizon.
Grant Watters is the clinical director of Mortimer Hirst Optometrists in Auckland. He has an interest in fitting and troubleshooting specialty contact lenses and is currently involved in a study of contact lens complications in keratoconus. He is also working alongside Paul Rose to develop new CL designs for keratoconus.