Spaceflight, blue-light-blocking lenses and diagnostic error in neuro-ophthalmology
Patient harm due to diagnostic error of neuro-ophthalmologic conditions
Stunkel L et al
Ophthalmology 2021; 128: 1356-1362
Review: A prospective study of 496 consecutive new adult patients seen at three neuro-ophthalmology clinics in the US between 2019 and 2020. The primary outcome was whether patients who were misdiagnosed before neuro-ophthalmology referral experienced harm as a result of the misdiagnosis. Referral diagnosis was incorrect or absent in 49% of cases. A total of 26% of misdiagnosed patients experienced harm as a result of misdiagnosis, which could have been prevented by earlier referral to neuro-ophthalmology in 97% of cases. Patients experienced inappropriate laboratory testing, diagnostic imaging, or treatment before referral in 23%. The most common reasons for referral were optic neuritis or optic neuropathy (23%), papilloedema (18%), diplopia or cranial nerve palsies (16%) and unspecified vision loss (11%).
The most common sources of diagnostic error were the physical examination (36%), generation of complete differential diagnosis (24%), history-taking (24%) and use or interpretation of diagnostic testing (13%). In 489 individuals (99%) the neuro-ophthalmic consultation had a direct impact on the patient’s care, with eight patients (2%) having their vision or life directly saved as a result of the assessment.
Comment: This study highlights the importance of prompt neuro-ophthalmic assessment for establishing correct diagnosis and instituting appropriate management which minimises harm to patients from excessive or inappropriate investigations and treatment. It also emphasises the value of neuro-ophthalmological assessment by a trained specialist in the diagnosis and management of potentially vision- and life-threatening conditions.
Optic nerve length before and after spaceflight
Wahlin A et al
Ophthalmology 2021; 128:309-316
Review: The study investigated whether microgravity during short- and long-duration missions to the International Space Station (ISS) can create deformations or movements of the eye or optic nerve, and if such changes can be linked to spaceflight-associated neuro-ocular syndrome (SANS), which manifests as blurred vision, optic disc oedema, globe flattening and choroidal folds.
Twenty-two astronauts underwent pre- and post-flight MRIs and their optic nerve parameters measured. Optic nerve length was shown to be increased by 0.8mm (p<0.001) following completion of the mission, primarily reflecting forward optic nerve head displacement by 0.63mm (p<0.001). This forward displacement was positively correlated with mission duration, pre-flight body weight and clinical manifestations of SANS.
Comment: Spaceflight-associated neuro-ocular syndrome poses one of the significant obstacles to piloted exploration of our immediate neighbours in the solar system, as the risk it poses to astronauts’ vision during planned long-duration flights, such as to Mars, is unknown. This study sheds light on possible mechanisms responsible for SANS and supports the view that it is caused by the altered pressure difference between the brain and the eye, leading to a forward push on the posterior part of the eye in microgravity. To further verify the theory, direct assessment of intracranial pressure in space would be required.
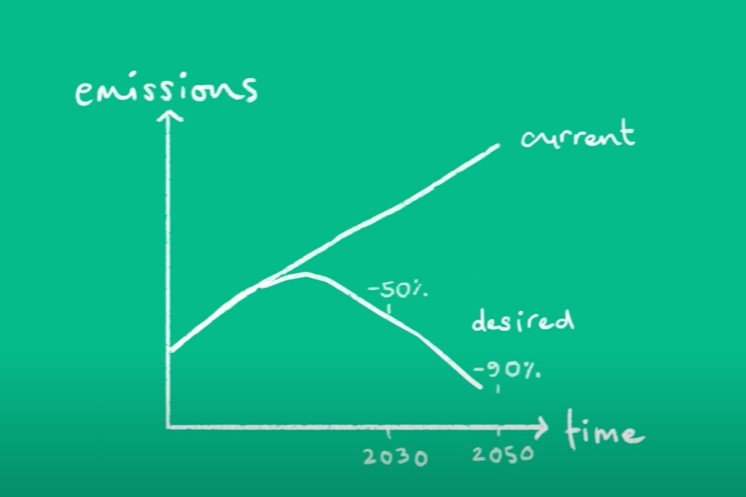
Do blue-light-blocking lenses reduce eye strain from screen time?
Singh S et al
Am J Ophthalmol 2021 Jun; 226:243-251
Review: A double-masked, randomised controlled trial investigating if blue-light-blocking (BLB) lenses are effective in reducing ocular signs and symptoms of eye strain associated with computer use. A total of 120 symptomatic computer users were randomised into a ‘positive’ or ‘negative’ advocacy arm (clinician either advocated or did not advocate the use of the lenses) and then further sub-randomised into BLB or non-filtering spectacles (four groups with 30 participants in each). Participants completed a two-hour computer task while wearing their assigned spectacles.
Primary outcome measures were the mean change in the eye strain symptom scores and critical flicker-fusion frequency (the frequency at which flickering light stops appearing to flicker and instead appears continuously illuminated – an objective measure of eye strain). The results revealed that BLB lenses did not alter signs or symptoms of eye strain with computer use compared to non-filtering lenses. Clinician advocacy type had no bearing on clinical outcome.
Comment: Eye strain with frequent and prolonged use of computers in modern society is extremely common. How the very weak emission of blue light (about 1,000-fold less than from natural daylight) from electronic devices can cause eye strain is unclear. It follows, therefore, that the mechanism by which BLB lenses are intended to relieve such strain is unclear. This study provides evidence that BLB lenses do not reduce eye strain associated with computer work, irrespective of whether or not they are advocated by a clinician.

Dr Taras Papchenko is a consultant ophthalmologist at Auckland Eye and Greenlane Clinical Centre, with sub-specialities in oculoplastics and neuro-ophthalmology. He graduated from Auckland Medical School in 2002 and was awarded a PhD in ophthalmology in 2013.