HZO-related disease post-cataract
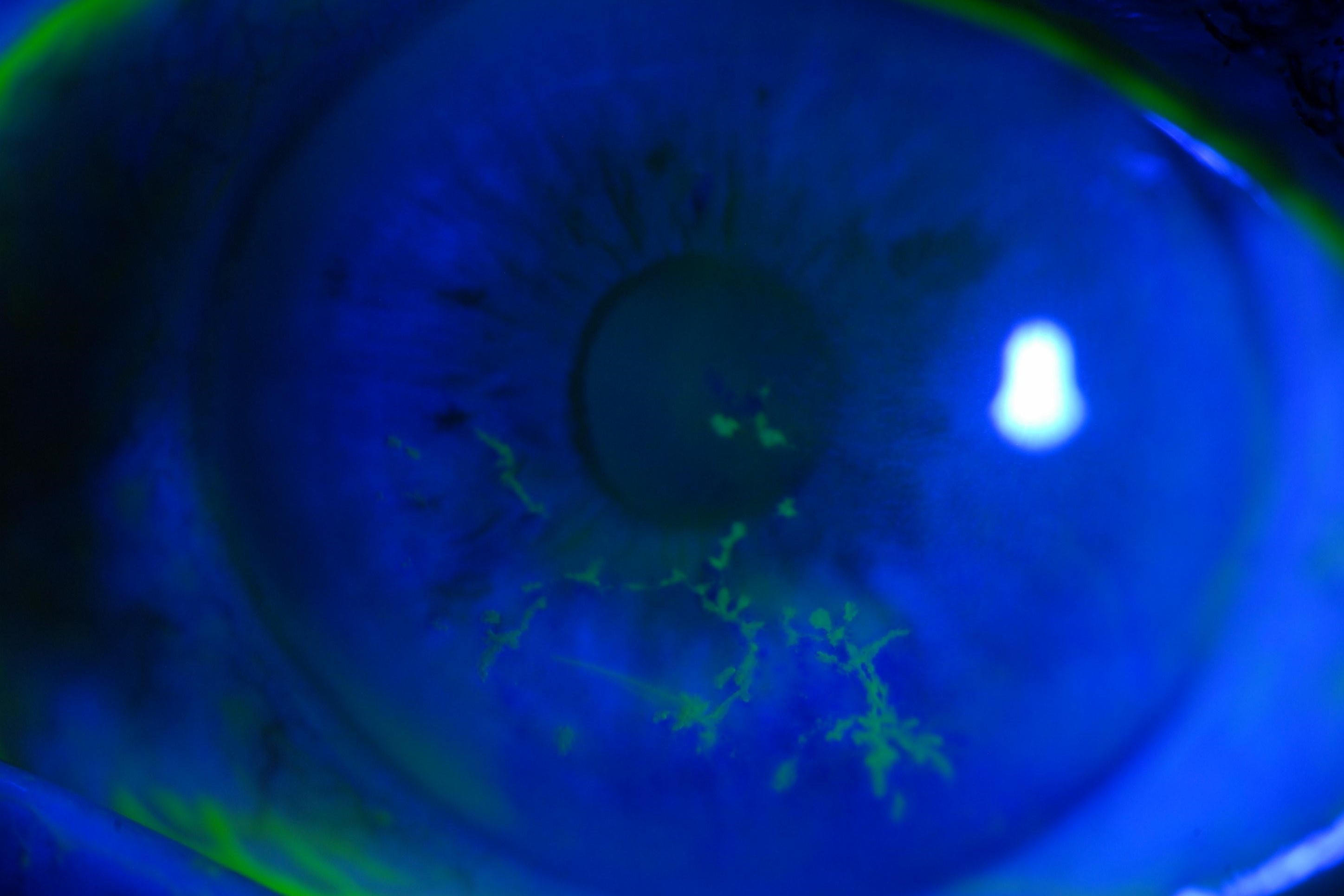
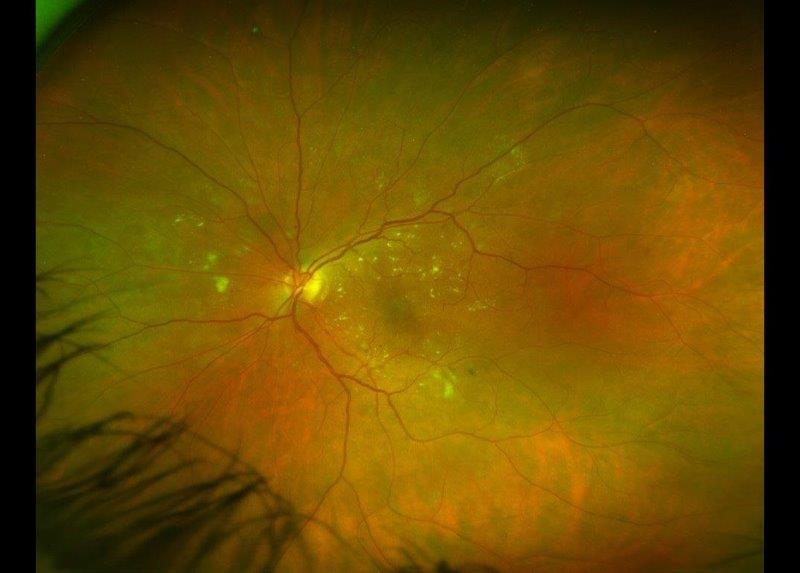
Herpes Zoster Ophthalmicus (HZO) is the reactivation of varicella zoster virus infection in the ophthalmic branch of the trigeminal nerve. Ocular complications of HZO include keratitis, uveitis, trabeculitis and, less commonly, optic neuritis and cranial nerve palsy. HZO can lead to chronic and recurrent ocular inflammation and secondary glaucoma.
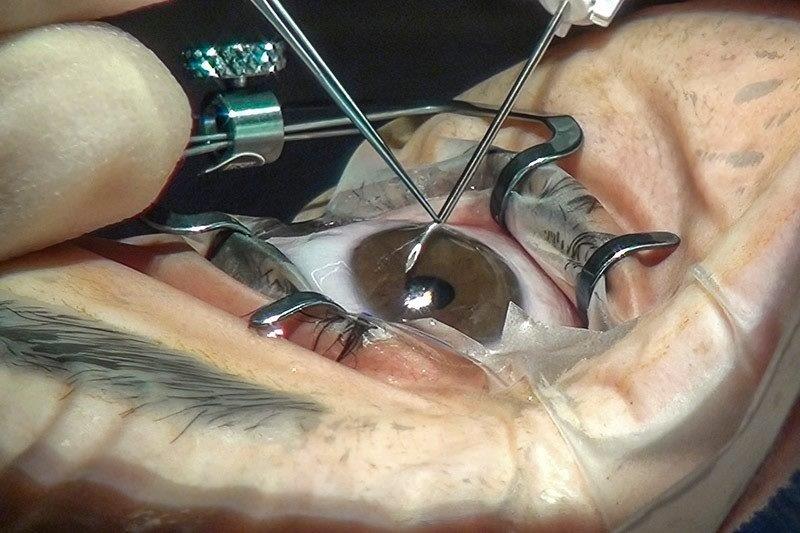
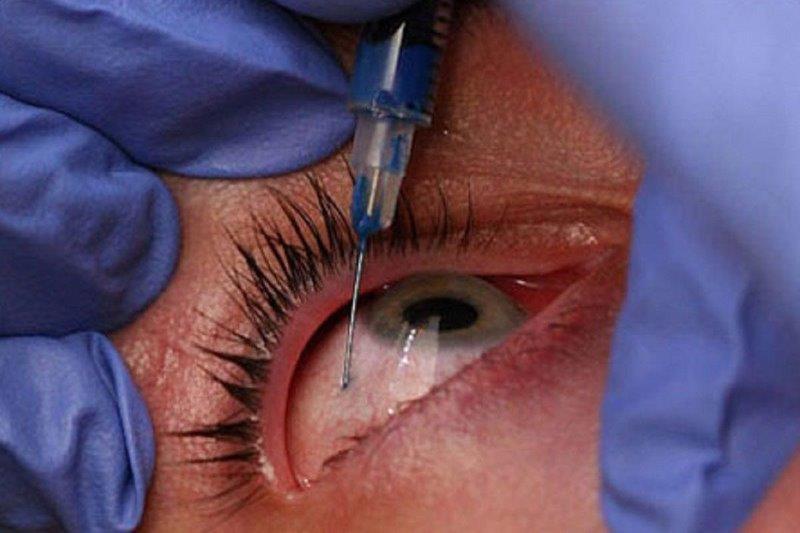
Cataract formation is common in eyes with HZO due to the combined effect of age, ocular inflammation and corticosteroid use. Cataract surgery in these patients can be complicated by the presence of corneal scarring, previous uveitis and recurrence of disease after surgery. However, little is known of the outcomes of cataract surgery in this group. Therefore, we carried out a retrospective review of patients undergoing cataract surgery after HZO, to evaluate the complications, visual outcomes and recurrence rates.
Overview and results
We identified 57 patients diagnosed with HZO keratitis or uveitis between 2005 and 2015 who subsequently underwent phacoemulsification cataract surgery in the affected eye. Thirty-eight patients (66.7%) had recurrent disease prior to surgery. Median time to surgery was 2.8 years. Thirty-two patients (56.1%) received pre-operative topical steroids, two received oral steroids and six received prophylactic oral acyclovir.
Intraoperative complications occurred in eight patients (14.0%) including: anterior capsule tear (n=3, 5.3%), posterior capsule tear (n=2, 3.5%) and iris prolapse (n=2, 3.5%). Postoperative complications included intraocular pressure (IOP) ≥ 30mmHg (n=2, 3.5%) and central corneal oedema (CMO) (n=8, 14.0%). CMO occurred in two patients (3.5%), which is equivalent to the rate reported in the Auckland Cataract Studies for routine cataracts at the Auckland District Health Board (ADHB).
HZO disease recurrence occurred in 40.4% post-surgery and was more common with shorter periods of quiescence (p=0.029) and with greater number of recurrences prior to surgery (p=0.039). Some patients had severe complications from recurrence of zoster-related ocular inflammation, including dislocation of intraocular lens, corneal decompensation requiring a corneal transplant and recurrent severe keratitis leading to evisceration. Overall visual outcomes were reasonable: median BCVA at 12 months post-op was 6/12, improved from a median of 6/30 pre-operatively. However, 12.3% of patients had poorer vision at 12 months post-op compared with their pre-op vision.
Comment
This study demonstrated that cataract surgery in eyes with a history of HZO keratitis or uveitis are more complex and carry a slightly increased risk of intraoperative and postoperative complications. Recurrence of ocular inflammation was common following surgery, particularly in the first year, and can lead to severe sequelae.
Clinicians should aim to maximize the period of quiescence prior to surgery (ideally, one year and a minimum of six months) to minimize the risk of recurrence. The role of antiviral therapy in the treatment and prevention of chronic/recurrent HZO is poorly understood and the Zoster Eye Disease Study (ZEDS) is currently underway in the United States to address this.
Until we have further guidance in this area, it is worthwhile considering antiviral prophylaxis perioperatively in patients with frequent or severe recurrences.
Reference:
Lu LM, McGhee CNJ, Sims JL, Niederer RL. High rate of recurrence of herpes zoster-related ocular disease after phacoemulsification cataract surgery. J Cataract Refract Surg. 2019 Jun;45(6):810-815. doi: 10.1016/j.jcrs.2019.01.003. Epub 2019 Apr 4.
Dr Lucy Lu is ophthalmology trainee based at Greenlane Clinical Centre in Auckland. She has recently completed a clinical research fellowship focusing on cornea and uveitis with the University of Auckland. Dr Rachel Niederer is a consultant ophthalmologist at the ADHB specialising in uveitis and medical retina, and has published extensively on uveitis, cornea and cataract surgery.