How Best disease patients keep seeing clearly
Duke Eye Centre researchers said they may have solved a decades-old mystery in ophthalmology, paving the way for a potential treatment of Best vitelliform macular dystrophy, or Best disease.
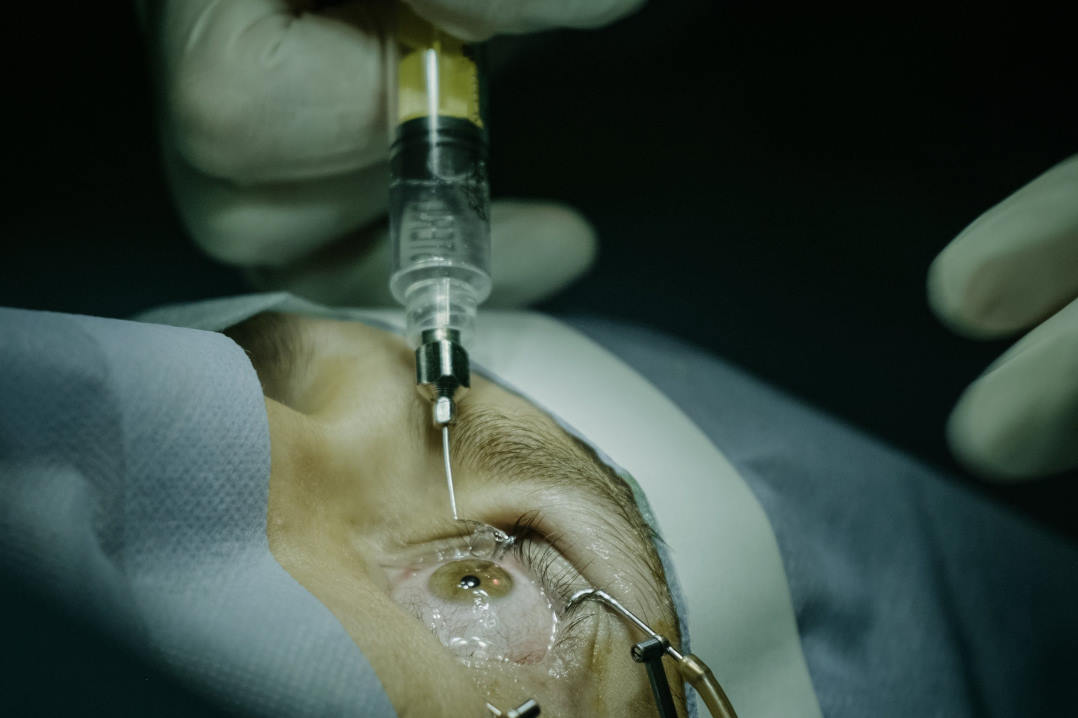
Patients with Best disease often continue to see clearly despite a large, egg-yolk-like deposit forming in the macula. The buildup pushes the light-sensing photoreceptors away from the support cells that keep them alive, a separation that, in theory, should severely damage eyesight. However, patients retain near-normal vision for years, even decades, said the Duke researchers.
“This has been a persistent conundrum in ophthalmology,” said Professor Vadim Arshavsky, who studies vitreoretinal diseases at Duke Eye Centre. “Using electron microscopy and three-dimensional electron tomography, we were able to uncover how this is possible.”
Working alongside Assistant Professors Tylor Lewis, University of Alabama at Birmingham, and Duke’s Oleg Alekseev, Prof Arshavsky’s team uncovered a surprise rescue system inside the eye.
When key retinal layers pull apart, the retinal pigment epithelium (RPE) sends out ultra-thin, thread-like extensions, called pseudopods. Writing in the Journal of Clinical Investigation, researchers said these pseudopods stretch across the widening gap, allowing support cells to keep doing the ‘daily cleanup’ and renewal work light-sensing cells need to survive and preserve vision. “These protrusions are very fine and difficult to detect, even with powerful microscopes, which is why they had gone undetected until now,” said Prof Arshavsky.
The researchers discovered the pseudopods while studying mice engineered to lack the ADAM9 gene. Although Best disease is caused by multiple gene mutations, the mice developed the same kind of enlarged space seen in human Best disease, yet their light-sensing cells kept functioning far longer than expected.
This discovery could inform new gene therapies now being tested for Best disease and similar conditions, said study lead A/Prof Lewis. “Understanding how the retina compensates on its own could help with the design of treatments that support or even strengthen this natural back-up system.”
Microscopic rescue mission
However, the team discovered that over time, perhaps when the deposits grow too large, the pseudopods dwindle. The mice’s photoreceptors began to degenerate, leading to vision loss.
“The RPE pseudopods we observed are about 5–10µ wide, roughly 10 times thinner than a human hair,” A/Prof Lewis said. “By comparison, vitelliform lesions in patients measure about 1mm, or 1,000µ. That means hundreds of these slender extensions would likely need to form within a single lesion to adequately support the photoreceptor cells beneath it.”
The structures also appear to be highly dynamic, constantly forming and retracting as they work to sustain large numbers of photoreceptors.
More studies are needed to learn how these pseudopods form and whether they appear in other eye diseases characterised by subretinal deposits that force cells apart, such as some forms of macular degeneration, said researchers.